Breast cancer screening relaunched
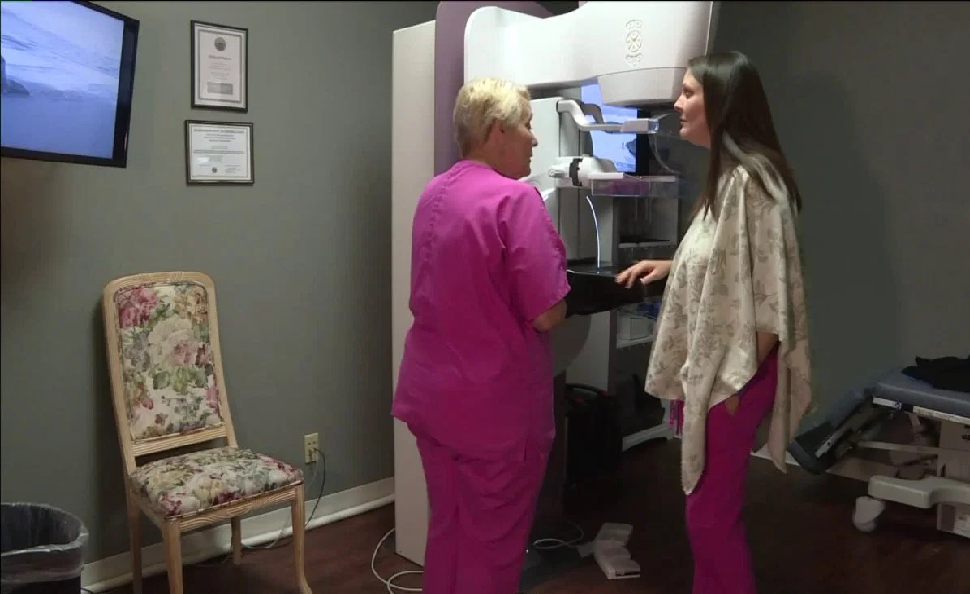
The National Cancer Institute, which is publishing a new 16-page document with the subtitle “Get informed and decide”, reaffirms the importance of systematic screening from the age of 50.
Only two out of three women invited to get tested for breast cancer do so . A semi-failure for public health because the assessment of the benefit / risk balance is more complex than some would like to believe.
“Better explain the benefits and risks of breast cancer screening ” is the ambition displayed by Professor Norbert Ifrah, president of the Cancer Institute (INCa), in a new document of 16 pages under -title “Get informed and decide”. This document will accompany the invitations to participate in the organized screening that the 9 million women aged 50 to 74 who will be affected will receive by mail.
This new document does not vary the recommendation to participate in screening, says Pr Ifrah immediately, it is a sharing tool between a woman and her attending physician.It is more complete than the previous leaflet, adds Dr Jérôme Viguier, in charge of the public health and care division of INCa. It contains information on the challenges and benefits, but also the risks and limits of screening: false positives, cancers diagnosed in the interval between two screening exams, over diagnosis and over treatment, radio-induced cancers …” Address all these questions is one of the merits of the brochure.
Regarding the risk, INCa recalls that: “out of 100 women aged 50, 3 will develop breast cancer within ten years.” Let us complete with the other figure which is important for considering her participation in a breast cancer program. screening, reduction of mortality. “International studies estimate that these programs make it possible to prevent between 15 and 21% of deaths from breast cancer,” we can read in the brochure. Translated into absolute risk, this means, as the INCa indicates on its website, that: “Between 150 and 300 deaths from breast cancer would be avoided per 100,000 women regularly participating in screening for 7 to 10 years.”
False positives, that is to say false alarming examinations, are the first consubstantial drawback to screening. It is even, specifies the INCa brochure, what happens “in most cases” when an anomaly is detected by mammography. In the end, additional examinations and anxiety will have been generated unnecessarily.
Another drawback, this time from mammograms themselves, is the risk of dying from radio-induced cancer, that is to say from cancer the appearance of which is due to repeated exposure to X-rays. details the brochure, “in the order of 1 to 10 per 100,000 women who have had a mammogram every 2 years for 10 years,” writes INCa.
It is also necessary to take into account the so-called “interval” cancers (between two mammograms) which will not be detected by systematic mammograms.